 
In patients older than 60 years who are less active and have comorbidities, hemiarthroplasty provides satisfactory function. However, mortality is reported to equalize at 1-year followup (RR = 1.04 95% 0.84-1.29). 
In more recent years, there has been an overall trend toward arthroplasty in the treatment of displaced femoral neck fractures, particularly in older patients, despite short-term increased mortality compared with internal fixation within the first 4 months (relative risk = 1.27 95% CI, 0.84-1.92). They found higher revision rates in the internal fixation group (42%) compared with the arthroplasty group (4%). 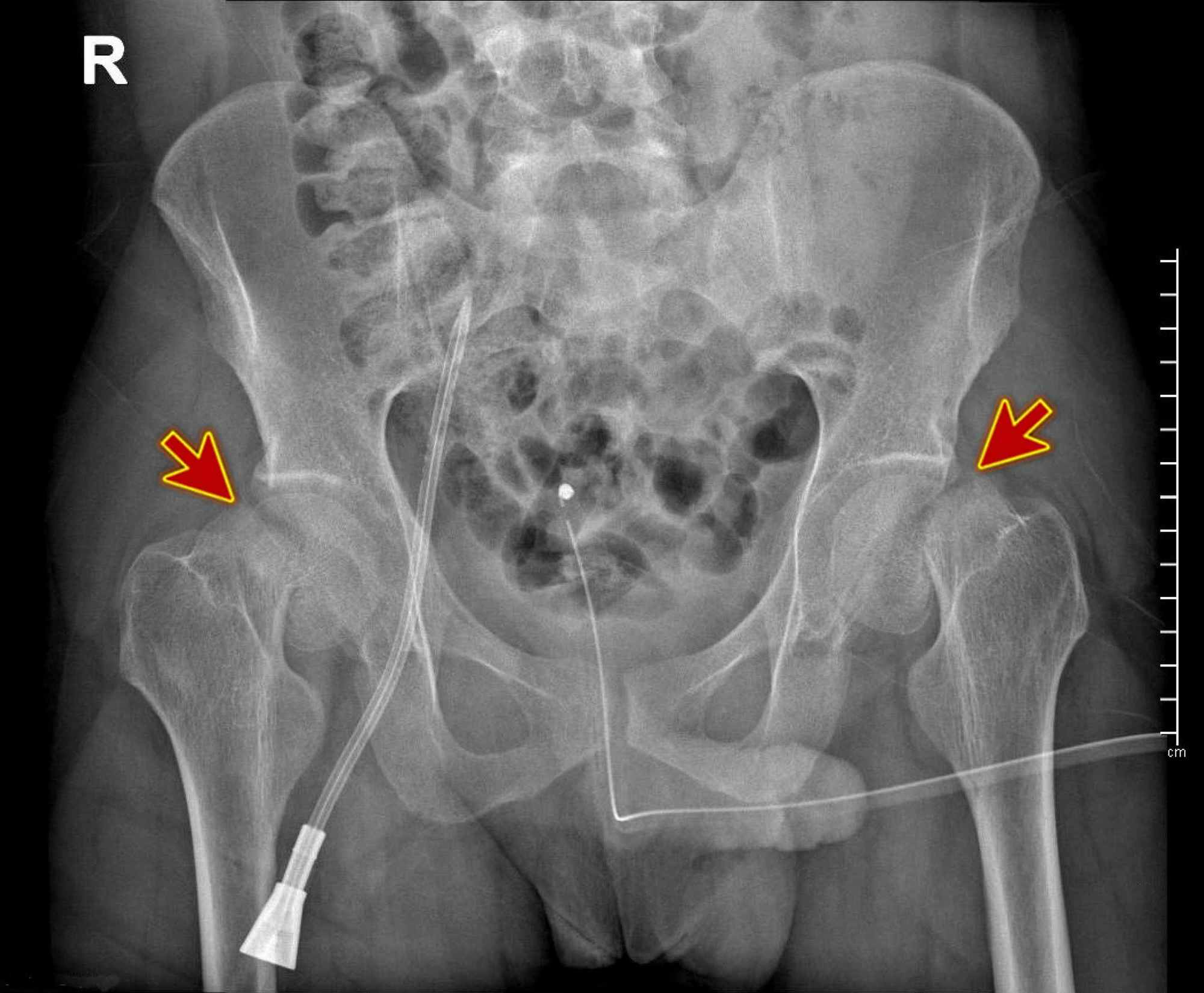
compared internal fixation and THA in healthy elderly patients with displaced femoral neck fractures. , in a meta-analysis, found a high incidence of nonunion (33%) and avascular necrosis (16%) after primary internal fixation of displaced femoral neck fractures. Arthroplasty often is used for displaced femoral neck fractures in the elderly while internal fixation is still favored in younger patients. Fixation options for displaced femoral neck fractures include hemiarthroplasty, THA, and internal fixation. Garden Types III and IV femoral neck fractures are displaced. However, there were no differences in reoperation rates between the two groups, leading to the study conclusion that both techniques were viable options in the treatment of nondisplaced femoral neck fractures. This study found that patients in the sliding hip screw group (9%) were significantly more likely to have avascular necrosis develop than patients in the cancellous hip screw group (5%). A recent prospective randomized multicenter study evaluated the rates of complications and reoperations for sliding hip screws and cancellous screw fixation in the treatment of nondisplaced femoral neck fractures. Internal fixation options include cannulated screws, dynamic hip screws, proximal femoral locking plates, and cephalomedullary nails. He therefore recommended that all Garden Types I and II nondisplaced fractures be fixed with internal fixation to allow for early weightbearing and provide stability without increasing the risk for avascular necrosis. Bentley looked at the treatment of impacted femoral neck fractures treated nonoperatively and found that these fractures displaced as much as 15% of the time. Internal fixation with preservation of the femoral head generally is favored for nondisplaced fractures of the femoral neck. Garden Types I and II femoral neck fractures are nondisplaced. The Garden classification is shown in the drawings and corresponding radiographs for Garden Types (A) I, (B) II, (C) III, and (D) IV femoral neck fractures. Types III and IV had lower union rates of 93% and 57% respectively. He found that Types I and II fractures had a 100% union rate. Gardens’ originally reviewed 80 patients with femoral neck fractures, which he classified in Types I to IV, and he followed these patients for at least 12 months postoperatively. The Garden classification incorporates displacement, fracture completeness, and relationship of bony trabeculae in the femoral head and neck. In 1961, Robert Symon Garden, a British orthopaedic surgeon with a focused interest in the femoral neck, described a more-comprehensive classification. An increase in vertical shearing forces results in higher risks of displacement, postreduction nonunion, and failure of fixation. As the angle of inclination increases, the forces transition from being compressive to shearing. The Pauwel classification, as it has come to be called, stratified fractures in three groups based on inclination of the fracture line relative to the horizontal: Type I, less than 30° Type II, 30° to 50° and Type III, greater than 50°. As reported by Bartonicek, it was only later in 1935 that a biomechanical classification was presented. įemoral neck fractures initially were classified by Sir Astley Cooper in 1823 as either intracapsular or extracapsular, which he felt had prognostic implications. In younger patients, high-energy trauma is responsible for most of these injuries. Fracture risk increases dramatically with age, with the majority of fractures occurring in older white women secondary to low-energy falls. There are many risk factors for femoral neck fractures, including female gender, low bone density, and reduced mobility. The incidence of femoral neck fractures in the United States is approximately 63.3 per 100,000 person/years in women and 27.7 per 100,000 person/years in men. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
